Why avoid ill-fitting shoes for foot health comfort
Most people assume uncomfortable shoes are simply an annoyance, yet wearing ill-fitting footwear causes serious medical complications beyond temporary discomfort. Tight shoes create pressure points leading to permanent deformities, whilst loose footwear destabilises your gait and strains muscles. Poor arch support triggers chronic conditions affecting your entire skeletal system. This guide explains the specific health risks of improper shoe fit and provides practical strategies to select footwear that protects your feet, joints, and overall mobility for years to come.
Table of Contents
- How Ill-Fitting Shoes Harm Your Foot Health
- The Biomechanical Impact Of Poor Shoe Fit
- Special Considerations: Ill-Fitting Shoes And Diabetic Foot Health
- Choosing And Maintaining Properly Fitting Shoes
- Explore Footwear Designed For Foot Health And Comfort
Key takeaways
| Point | Details |
|---|---|
| Friction damage | Tight or loose shoes cause blisters, calluses, corns, and ingrown toenails through constant rubbing. |
| Structural deformities | Narrow footwear contributes to bunions, hammertoes, and neuromas by compressing foot bones. |
| Systemic joint pain | Poor shoe fit alters gait patterns, creating stress on knees, hips, and lower back. |
| Diabetic complications | Ill-fitting shoes dramatically increase ulceration risk in people with diabetes due to pressure and neuropathy. |
| Replacement timing | Shoes lose supportive properties after 300-500 miles, requiring regular replacement to maintain foot health. |
How ill-fitting shoes harm your foot health
Your feet contain 26 bones, 33 joints, and over 100 muscles working together to support your entire body weight. When shoes don’t fit properly, this intricate system faces constant stress that manifests as immediate discomfort and long-term damage. Understanding these specific mechanisms helps you recognise warning signs before minor irritation becomes chronic disability.
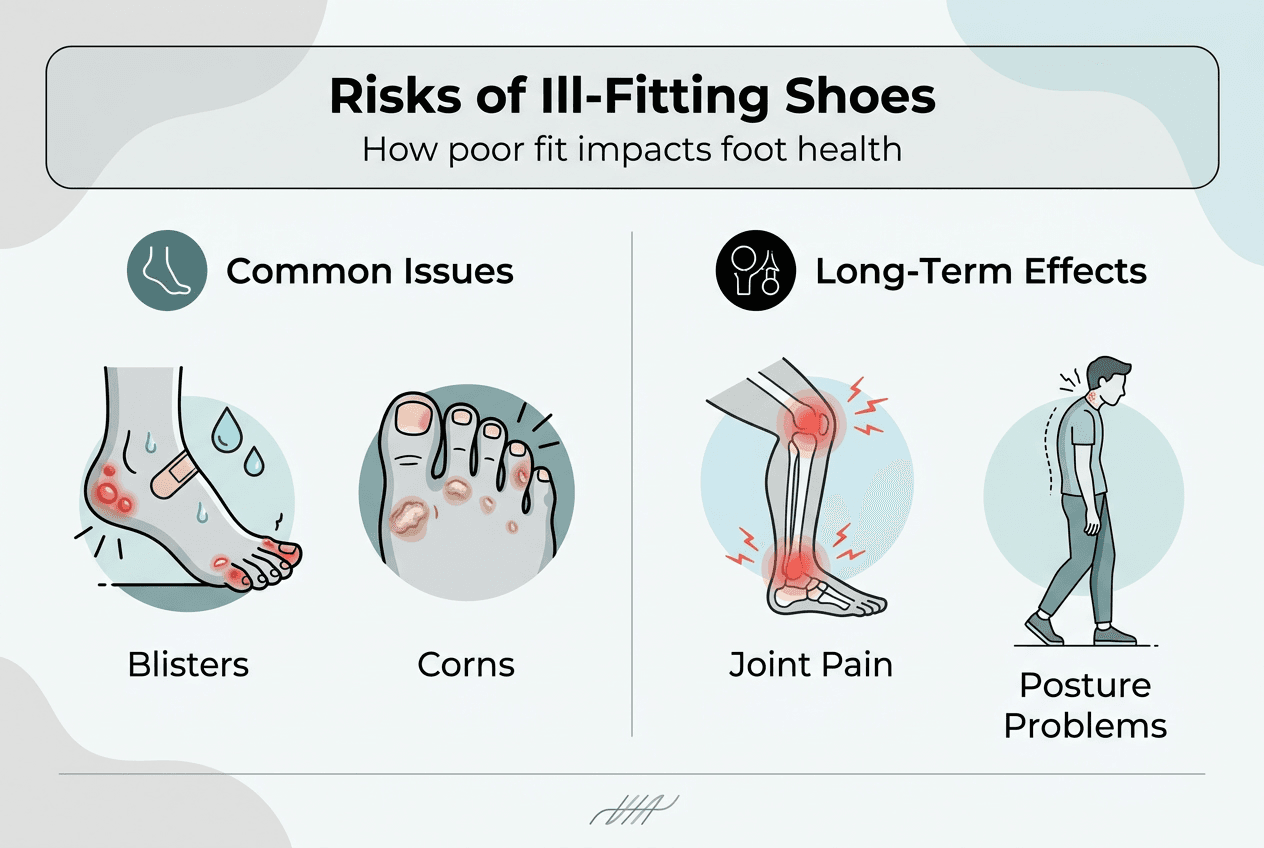
Tight shoes create friction leading to blisters, calluses, corns, and ingrown toenails. The constant rubbing between skin and material generates heat and pressure that separates skin layers, forming fluid-filled pockets. Repeated trauma thickens skin into painful calluses whilst compressing toenails into surrounding flesh. Narrow toe boxes squeeze bones together, gradually pushing your big toe towards neighbouring digits and creating the bony protrusion characteristic of bunions.
Loose footwear presents equally serious risks through instability causing ankle sprains and chronic muscle fatigue. When shoes slide around your feet, your toes automatically grip to prevent slippage. This constant clenching exhausts small foot muscles and strains tendons connecting to your lower leg. The lack of secure heel contact allows excessive movement during walking, increasing your vulnerability to rolling ankles on uneven surfaces.
Pro Tip: Check for red marks or indentations on your feet after removing shoes. These pressure points indicate areas where footwear is too tight and causing tissue damage.
Insufficient arch support creates one of the most debilitating footwear-related conditions. Your plantar fascia, a thick band of tissue running along your foot’s bottom, absorbs shock with each step. Shoes lacking proper arch contours force this ligament to overstretch, causing microscopic tears that inflame into plantar fasciitis. Morning heel pain becomes the hallmark symptom as the fascia tightens overnight then tears again with your first steps.
“The cumulative effect of wearing poorly fitted shoes transforms minor discomfort into permanent structural changes requiring medical intervention.”
Common foot ailments directly attributable to improper fit include:
- Metatarsalgia: ball-of-foot pain from excessive pressure on forefoot bones
- Morton’s neuroma: nerve thickening between toes causing burning sensations
- Achilles tendinitis: inflammation from heel counter rubbing or poor ankle support
- Stress fractures: tiny bone cracks from repetitive impact without adequate cushioning
These conditions don’t develop overnight. Months or years of subtle damage accumulate until pain becomes constant. Why shoe fit matters extends beyond comfort to preventing irreversible skeletal changes that limit your mobility and activity choices throughout life.
The biomechanical impact of poor shoe fit
Your walking pattern represents a complex chain reaction starting at ground contact and travelling through your entire skeletal system. Shoes act as the interface controlling how forces transmit upward, making proper fit essential for maintaining healthy biomechanics. When footwear distorts natural movement patterns, compensatory changes ripple through joints far above your feet.
Ill-fitting shoes fundamentally alter gait causing knee, hip, and back pain whilst restricting circulation. Your body instinctively adjusts stride length, foot strike angle, and weight distribution to accommodate uncomfortable footwear. These modifications seem minor initially but create abnormal stress concentrations in joints designed for different loading patterns. Over time, cartilage wears unevenly, ligaments stretch asymmetrically, and muscles develop imbalances that manifest as chronic pain.
The mechanical relationship between shoe fit and body alignment follows predictable patterns:
- Tight footwear increases pressure and shear forces, compressing blood vessels and nerves whilst creating friction hotspots
- Loose shoes reduce stability, forcing ankle and knee joints to work harder maintaining balance during each step
- Poor arch matching strains the plantar fascia, triggering inflammation that radiates up the posterior chain
- Inadequate heel cushioning transmits shock directly into knee cartilage, accelerating degenerative joint disease
- Elevated heels shift your centre of gravity forward, increasing lumbar spine curvature and lower back muscle tension
Circulation problems represent another serious consequence often overlooked until symptoms become severe. Tight shoes compress blood vessels running along your foot’s top and sides, reducing oxygen delivery to tissues. You might notice numbness, tingling, or coldness in your toes after wearing constrictive footwear for several hours. Chronic compression can damage nerves permanently, creating persistent sensory disturbances even when barefoot.
“Biomechanical compensation for poor shoe fit creates a cascade of musculoskeletal problems that extend well beyond the initial point of discomfort.”
Your knees particularly suffer from footwear-induced gait changes. When shoes lack proper support, your feet roll inward excessively during walking, a motion called overpronation. This internal rotation transmits up your shin, forcing your knee to twist with each step. The repetitive torque strains ligaments and irritates cartilage surfaces, accelerating arthritis development. Similarly, shoes causing underpronation concentrate impact forces on your knee’s outer compartment.

Understanding shoe fit and foot biomechanics empowers you to recognise how seemingly minor footwear choices affect your entire body. Comfort footwear features specifically address these biomechanical requirements, providing the structural support necessary to maintain natural movement patterns and prevent compensatory damage throughout your kinetic chain.
Special considerations: ill-fitting shoes and diabetic foot health
Diabetes creates unique vulnerabilities that transform ordinary footwear mistakes into medical emergencies. Elevated blood sugar levels damage nerves and blood vessels, reducing sensation and healing capacity in your feet. What might cause temporary discomfort in others can progress to serious ulcers requiring hospitalisation or amputation in diabetic individuals. Understanding these heightened risks makes proper shoe fit absolutely critical for managing diabetic foot health.
People with diabetes face dramatically increased ulceration risk from ill-fitting footwear due to uneven pressure distribution and peripheral neuropathy. Nerve damage prevents you from feeling pressure points, blisters, or cuts developing inside your shoes. Simultaneously, poor circulation slows healing, allowing minor injuries to become infected wounds. Research examining diabetic patients found 0% wore optimal footwear, with wider feet and existing ulcers correlating strongly with inappropriate shoe selection.
Diabetic footwear requirements differ substantially from standard shoe considerations:
| Feature | Standard shoes | Diabetic requirements | Health benefit | | — | — | — | | Width | Regular or wide | Extra-wide with adjustable closures | Eliminates pressure points on bony prominences | | Interior | Standard seams | Seamless or padded lining | Prevents friction creating skin breakdown | | Insole | Basic cushioning | Soft, moulded orthotics | Distributes pressure evenly across entire foot | | Back design | Varied styles | Closed heel counter | Protects vulnerable Achilles area from rubbing | | Depth | Standard | Extra depth for custom inserts | Accommodates foot deformities without compression |
Pro Tip: Inspect the inside of your shoes daily by running your hand along all surfaces. Even small wrinkles or debris can create pressure points leading to ulcers when neuropathy prevents feeling the irritation.
Diabetic foot footwear must incorporate extra-wide sizing, soft insoles, and avoid open-back styles to prevent complications. The extra width accommodates swelling and deformities common in diabetic feet without creating constriction. Soft, cushioned insoles made from materials like plastazote mould to your foot’s unique contours, eliminating high-pressure zones that damage tissue. Closed-back designs protect your heel and Achilles tendon from friction whilst providing stability that prevents falls.
Regular foot examinations become essential when selecting footwear. Check for redness, swelling, temperature changes, or skin breakdown after wearing new shoes for even short periods. These warning signs indicate improper fit before serious damage occurs. Shoe fit for diabetics requires professional assessment to identify specific risk factors like prominent metatarsal heads, hammer toes, or previous ulcer sites needing accommodation.
The financial and health costs of diabetic foot complications make investing in proper footwear remarkably cost-effective. Ulcers often require months of wound care, antibiotics, and potential surgery, whilst proper shoes prevent most cases entirely. Diabetic footwear selection should involve podiatric consultation to ensure your shoes meet medical-grade standards for protection and support.
Choosing and maintaining properly fitting shoes
Selecting footwear that truly fits requires more than trying shoes on and walking around the shop briefly. Your feet change size throughout the day, between left and right sides, and over your lifetime. Systematic measurement and evaluation ensure you purchase shoes providing optimal support and comfort for years of wear.
Timing your shoe shopping affects fit accuracy significantly. Measure feet late in the day to account for natural swelling that occurs from standing and walking. Your feet can expand up to half a size by evening, making morning measurements misleading. Shoes fitting perfectly at 9am might feel uncomfortably tight by afternoon, creating the pressure problems discussed earlier.
Professional fitting techniques provide objective data beyond subjective comfort:
- Use a Brannock device to measure both length and width accurately, checking each foot separately since asymmetry is common
- Ensure thumb-width space between your longest toe and shoe end when standing, allowing room for forward foot movement during walking
- Check heel fit by sliding one finger between your heel and shoe counter; snug contact without slippage indicates proper sizing
- Walk on hard surfaces wearing both shoes to assess arch support, cushioning, and overall stability during natural movement
- Verify the widest part of your foot aligns with the shoe’s widest point, preventing compression of metatarsal heads
Pro Tip: Always try shoes with the socks or orthotics you’ll actually wear. Thickness variations dramatically affect fit, and testing with thin dress socks when you’ll wear thick athletic socks guarantees sizing problems.
Replacing shoes at appropriate intervals maintains the supportive properties protecting your feet. Even high-quality footwear loses cushioning and structural integrity after 300-500 miles of use. Midsole foam compresses permanently, arch support flattens, and heel counters break down. These changes occur gradually, making deterioration difficult to notice until pain develops. Track your shoe mileage or replace annually if you wear them daily.
The cushioning versus support debate affects shoe selection based on your foot type. Excessive cushioning reduces sensory feedback and can weaken foot muscles over time, whilst insufficient padding transmits harmful impact forces. Neutral feet benefit from moderate cushioning with arch support, flat feet require motion control features preventing overpronation, and high arches need extra shock absorption compensating for reduced natural cushioning.
Maintenance practices extend shoe life whilst preserving fit:
| Maintenance task | Frequency | Purpose |
|---|---|---|
| Air dry after wear | Daily | Prevents moisture breakdown of materials |
| Rotate between pairs | Every other day | Allows midsole foam to recover compression |
| Clean exterior | Weekly | Removes debris that can create pressure points |
| Inspect interior | Monthly | Identifies worn areas needing replacement |
| Replace insoles | Every 3-6 months | Restores cushioning and arch support |
Footwear selection guide principles apply across all shoe types, from athletic trainers to dress shoes. Prioritise fit over fashion, recognising that temporary style preferences matter far less than long-term foot health. Learning to evaluate shoe technology helps you identify genuinely supportive features versus marketing claims lacking biomechanical benefit.
Explore footwear designed for foot health and comfort
Finding shoes that combine proper fit with advanced support technology transforms your daily comfort and long-term mobility. After understanding how ill-fitting footwear damages your feet, joints, and overall biomechanics, the logical next step involves selecting shoes specifically engineered to prevent these problems.
YDA UK specialises in footwear that prioritises both health and style, offering shoes for problem feet incorporating advanced biomechanical design. The YDA shoe collection addresses specific conditions like diabetic foot complications, plantar fasciitis, and general mobility concerns through evidence-based construction methods. Each design integrates proper arch support, pressure-distributing insoles, and anatomically correct toe boxes that accommodate natural foot shape without compression. Explore the technology of YDA shoes to understand how innovative materials and engineering principles create footwear that actively supports your foot health rather than compromising it.
FAQ
How can I tell if my shoes really fit well?
Proper fit feels snug through the midfoot and heel without creating pressure points or allowing excessive movement. You should have approximately thumb-width space between your longest toe and the shoe’s end when standing. Check that you can wiggle all toes freely and that the widest part of your foot aligns with the shoe’s widest section. No heel slippage should occur when walking, and you shouldn’t feel any pinching, rubbing, or numbness after wearing shoes for 30 minutes.
Can wearing high heels cause long-term foot problems?
High heels significantly increase injury risk, with studies showing 3.8 times higher odds of ankle sprains when worn over four hours whilst standing. They shift your body weight forward onto the forefoot, compressing metatarsal bones and straining the Achilles tendon. Prolonged use shortens calf muscles, alters natural gait mechanics, and accelerates arthritis development in the ball of your foot. Limiting heel height to under 5cm and duration to special occasions helps minimise these cumulative effects.
What special features should diabetic footwear have?
Diabetic shoes require extra width to accommodate swelling and deformities without creating pressure points that could ulcerate. Soft, seamless interiors prevent friction against vulnerable skin, whilst cushioned insoles distribute weight evenly across your entire foot. Closed-back designs protect the heel area from rubbing, and adjustable closures like Velcro straps allow customised fit as foot dimensions fluctuate. Features of diabetic footwear should include adequate depth for custom orthotics and non-slip soles preventing falls that could injure neuropathic feet.
How often should I replace my shoes to maintain foot health?
Replace shoes every 300-500 miles or when visible signs of wear appear, such as compressed midsoles, worn tread patterns, or broken-down heel counters. Athletic shoes used daily typically need replacement every 6-8 months, whilst dress shoes worn occasionally may last several years. The cushioning and support structures degrade gradually even without obvious exterior damage. Shoe replacement advice emphasises monitoring for decreased comfort, new foot pain, or reduced shock absorption as indicators that supportive properties have deteriorated beyond effectiveness.
Recommended
- Workflow for Finding Right Shoes for Health and Comfort – YDA UK
- Why Shoe Fit Matters for Foot Health and Comfort – YDA UK
- Footwear Selection Guide 2025: Choose Shoes for Health and Comfort – YDA UK
- 7 Examples of Foot Health Shoes for Everyday Comfort – YDA UK
- Post-Stroke Foot Drop Brace – Corrective AFO Orthosis | FLEX-AFO
